As spring arrives on the Costa del Sol, many people make a familiar swap: supportive footwear gets traded for lighter shoes and flip-flops. Whilst this feels wonderful in the sunshine, it often brings one of the most common complaints back into clinic – plantar fasciitis.
At Costa Health, we regularly see patients from Mijas and Marbella struggling with this condition. Without proper management, it can become surprisingly painful and start to affect daily life.
What Is Plantar Fasciitis?
Plantar fasciitis is irritation of the plantar fascia, a thick band of connective tissue that runs along the bottom of your foot, connecting your heel to your toes.
Its role is to support the arch of the foot and absorb load during walking and activity. When this tissue becomes overloaded or strained, it leads to pain most commonly felt at the heel.
Why Does It Happen?
Plantar fasciitis is typically a load-related issue rather than a sudden injury. Spring is a key trigger period, as activity levels increase and footwear support decreases at the same time.
Common contributing factors include:
- A sudden increase in walking or physical activity
- Switching to unsupportive footwear such as flip-flops
- Tight calves or reduced ankle mobility
- Poor foot biomechanics
- Standing for long periods, particularly on hard surfaces
- Increased load through sport or lifestyle changes
Typical Symptoms
The most recognisable sign of plantar fasciitis is sharp heel pain with those first few steps in the morning. Other common symptoms include:
- Pain after periods of rest, such as getting up from a chair
- Discomfort that eases slightly with movement but returns after prolonged activity
- Tenderness along the underside of the heel
Managing Plantar Fasciitis at Home
Early management can make a significant difference. The following strategies are a good starting point:
Choose Supportive Footwear
Avoid completely flat shoes and unsupportive flip-flops. Look for footwear with arch support and adequate cushioning, particularly for daily walking.
Stretch Your Calves Daily
Tight calf muscles place additional strain on the plantar fascia. A consistent stretching routine is one of the most effective self-management tools available.
Quick Tip: Try a simple calf stretch against a wall each morning before you take your first steps. Hold for 30 seconds on each side to reduce that sharp first-step stiffness.
Manage Your Load
Temporarily reduce excessive walking or prolonged standing, especially on hard surfaces. This does not mean stopping activity altogether – it means being mindful of how much load you are placing on the tissue while it recovers.
Strengthen Your Feet
Simple foot strengthening exercises can improve long-term support and reduce the likelihood of recurrence. Our physiotherapy team can guide you through an appropriate programme.
Use Ice or Self-Massage
Rolling your foot over a cold bottle or massage ball for a few minutes can help reduce irritation and provide short-term relief between appointments.
When to Seek Professional Treatment
If symptoms persist beyond a few weeks, or begin to limit your daily activity, a professional assessment is important. Plantar fasciitis can become a chronic condition and considerably more difficult to manage if left unaddressed.
At Costa Health, our physiotherapy team in Mijas and Marbella assesses each case individually, looking at biomechanics, movement patterns, and contributing factors to create a targeted treatment plan. This is the same patient-centred approach we take with other load-related conditions, such as knee pain during running and exercise or meniscus injuries.
Shockwave Therapy for Persistent Plantar Fasciitis
For cases that have not responded to conservative management, shockwave therapy is one of the most effective treatment options available.
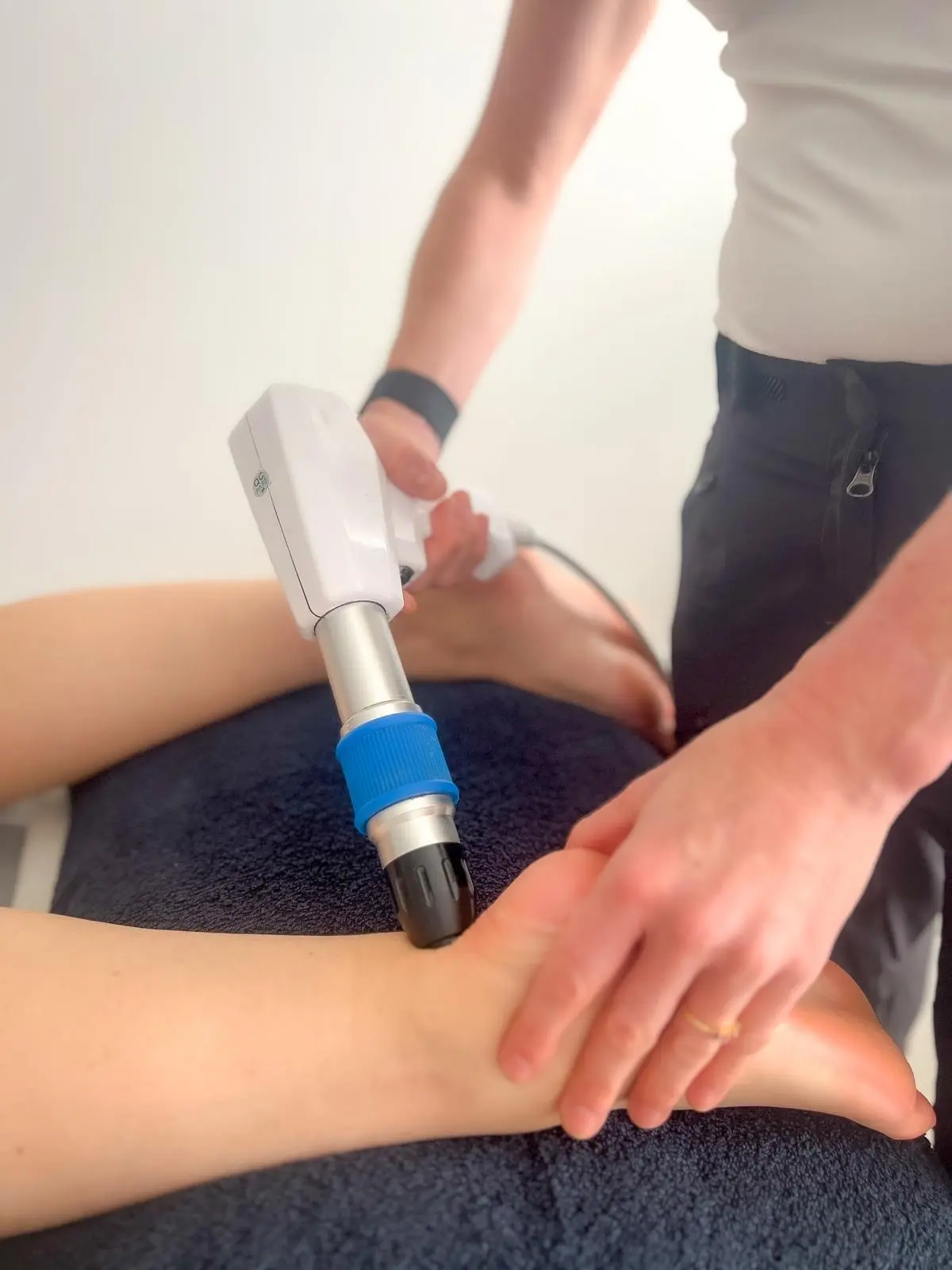
How Does It Work?
Shockwave therapy delivers controlled acoustic waves into the affected tissue. This stimulates a healing response by increasing blood flow, promoting tissue repair, and reducing pain sensitivity.
Why Is It Effective?
Plantar fasciitis is often a chronic overload condition in which the tissue has struggled to heal properly on its own. Shockwave therapy helps restart this healing process and is particularly effective in long-standing cases. It is safe, evidence-based, and requires no injections or medication.
Quick Tip: A typical course is three to six sessions. Many patients notice improvement within the first two to three treatments, though individual responses vary depending on the duration and severity of the condition.
What Shoes Should You Wear This Spring?
Footwear choice is one of the simplest and most effective ways to protect your plantar fascia as the weather warms up. We recommend:
- Supportive trainers for daily walking
- Sandals with built-in arch support
- Limiting time in completely flat flip-flops, particularly on prolonged walks or hard surfaces
If you prefer lighter footwear during the warmer months, try alternating with more supportive options throughout the day rather than wearing unsupportive shoes for extended periods.
If you are also active in sport this spring, whether running, cycling, or on the golf course it is worth reading about common golf and sports injuries on the Costa del Sol to keep your whole body moving well alongside your feet.
Frequently Asked Questions
How long does plantar fasciitis last?
Duration varies depending on severity and how early treatment begins. Some cases resolve within a few weeks with good self-management; others can persist for several months if left unaddressed. Early assessment and treatment significantly improve outcomes.
Is it OK to keep walking with plantar fasciitis?
Yes, but load management is important. Moderate walking is generally fine; however, if your pain is worsening with activity, reducing the amount and intensity of walking temporarily is advisable. A physiotherapist can help you find the right balance for your situation.
Will plantar fasciitis go away on its own?
Some mild cases do improve with rest and footwear changes alone. However, many cases become persistent or recurrent without targeted treatment. Seeking professional advice early gives you the best chance of a full and lasting recovery.
Is shockwave therapy painful?
Shockwave therapy can cause some discomfort during the session, but most patients find it well tolerated. Each session is short, and any post-treatment soreness typically settles quickly.
How many shockwave therapy sessions are needed for plantar fasciitis?
A typical course is three to six sessions, depending on the severity and how long the condition has been present. Your physiotherapist will advise on the most appropriate number of treatments following your initial assessment.