Being told you have a disc bulge or disc herniation can be alarming. Many patients arrive at Costa Health worried that their back is permanently damaged, that the disc will “slip” further, or that surgery is inevitable. The reassuring truth is this: most disc bulges and disc herniations do not require surgery, and the vast majority improve significantly with the right guidance, movement strategies, and rehabilitation.
Flora, our physiotherapist and low back pain specialist, combines advanced physiotherapy techniques with spinal mobilisation skills to treat disc-related injuries and sciatica. In this Ask the Expert article, she explains what disc injuries really mean, why symptoms occur, and how recovery works.
What Is a Disc Bulge or Herniation?
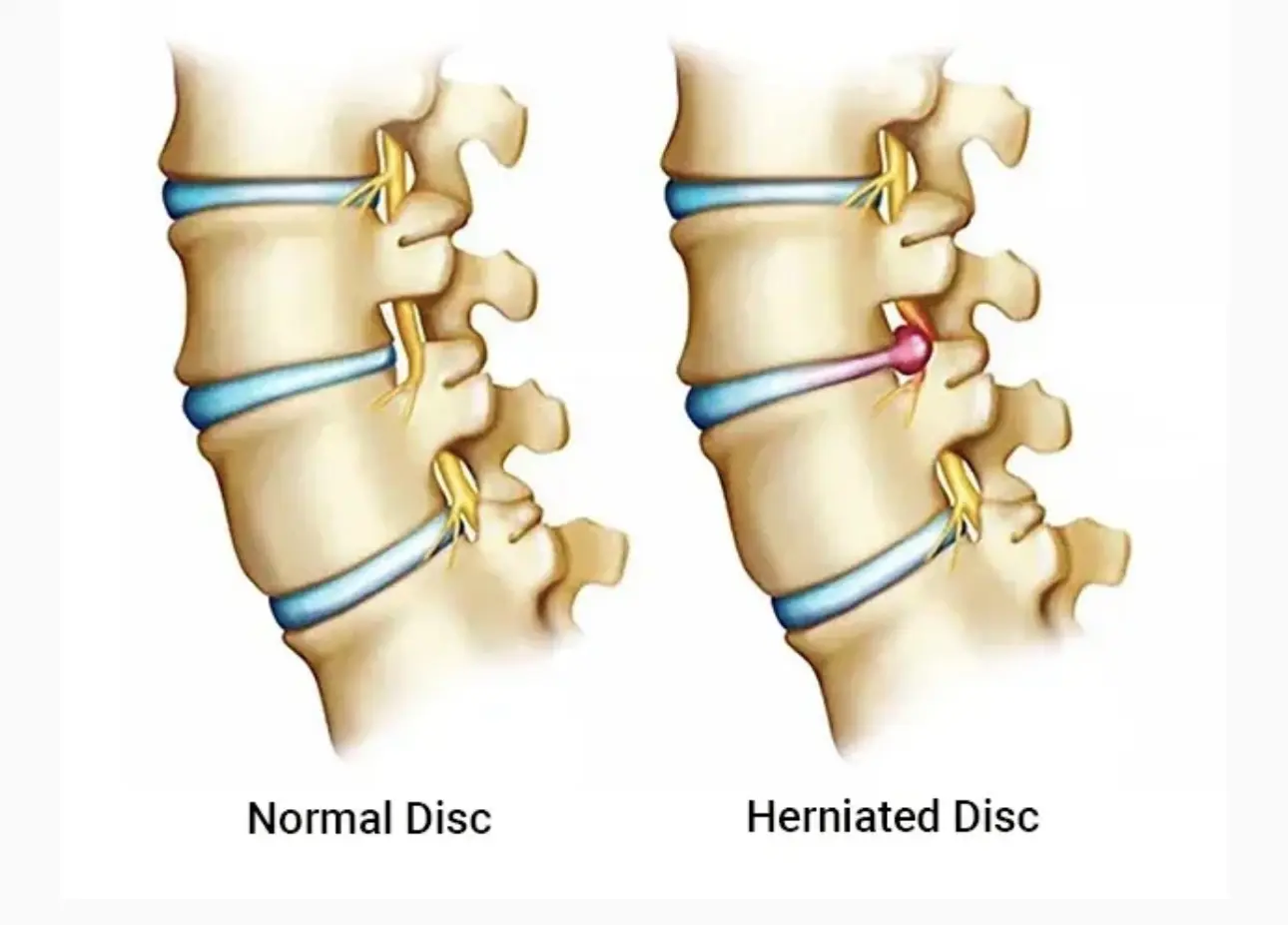
Between each vertebra sits a spinal disc, a strong, flexible cushion that absorbs pressure and allows you to bend, twist, and move freely. A disc bulge or herniation occurs when part of the disc pushes outward. This is extremely common and is often a normal part of ageing.
Disc Bulge
- The disc has changed shape slightly
- The outer layers remain intact
- Symptoms range from none at all to mild or moderate discomfort
Disc Herniation
- The inner part of the disc has pushed further outward
- It may irritate or press on a nearby nerve root
- Symptoms can include sciatica, leg pain, or numbness
Crucially, a disc bulge does not automatically cause pain. MRI findings frequently do not match symptoms, which is why a thorough clinical assessment matters far more than a scan result alone. If you are wondering whether you need imaging, our guide on whether you need an MRI or X-ray for back or neck pain explains what to expect.
Why Disc Problems Cause Pain
Disc-related back pain can arise through several overlapping mechanisms:
- Inflammation around the disc
- Local chemical irritation from disc material
- Pressure on a nerve root
- Muscle spasm protecting the area
- Restricted movement due to pain or guarding
When a nerve is irritated, symptoms can travel into the leg and include:
- Leg pain or sciatica
- Tingling or numbness
- Shooting or burning sensations
- Weakness in specific movements
These symptoms can be worrying, but they are all treatable. Understanding the underlying mechanism helps us select the right treatment approach from the outset.
Do Disc Bulges Heal on Their Own?
Yes, in most cases. The body is highly effective at reducing inflammation, reabsorbing disc material, and calming nerve irritation. Multiple studies confirm that disc herniations shrink over time, even without surgical intervention.
This is not an entirely passive process, however. The right movement strategies and guided rehabilitation accelerate recovery considerably and help prevent recurrence.
Quick Tip: Staying gently active during recovery is far better than complete rest. Prolonged bed rest increases stiffness and slows healing. Your physiotherapist can identify which movements are safe and helpful for your specific pattern of pain.
Why Surgery Is Rarely Required
Surgery is considered only in a small minority of cases, specifically when:
- There is progressive muscle weakness
- There is loss of bowel or bladder control (a medical emergency requiring immediate attention)
- Severe, unrelenting pain has not responded to several weeks of appropriate care
- There is confirmed nerve compression affecting daily function
These situations represent a small fraction of disc injury presentations. The vast majority of patients recover fully through:
- Correct movement strategies
- Spinal mobility work
- Load management
- Targeted strengthening
- Gradual return to normal activity
How Flora Assesses Disc Injuries
A thorough assessment is the foundation of effective treatment. During your appointment, Flora will identify:
- Which movements worsen or relieve your symptoms
- Whether nerve tension is involved
- Whether the disc is inflamed or irritated
- How the pelvis, hips, and thoracic spine are contributing
- Whether weakness or stiffness is a factor
Because Flora’s training spans both physiotherapy and spinal mobilisation, she can address joint restrictions, muscle imbalances, and nerve irritation within one cohesive treatment plan, rather than requiring referrals between multiple practitioners.
How Disc-Related Pain Is Treated at Costa Health
1. Reducing Disc Irritation
Repeated extension movements, side-glides, or gentle flexion work can reduce pressure on the disc and calm nerve irritation. The specific approach depends entirely on your movement pattern; there is no one-size-fits-all protocol.
2. Managing Nerve Pain
Specific mobilisation techniques and nerve-gliding exercises help reduce leg symptoms. When performed correctly, these are gentle yet highly effective for reducing referred pain and numbness.
3. Restoring Spinal Mobility
When certain spinal joints are stiff, neighbouring segments compensate and become overloaded. Mobilisation and manipulation techniques restore natural movement and reduce strain on the irritated disc.
4. Targeted Strengthening
Weak gluteal muscles, reduced deep stabiliser activity, or poor hip strength all place extra stress on the lower back. A progressive strengthening programme is essential for lasting recovery and preventing recurrence.
5. Hip and Pelvic Control
Improving hip mobility and control reduces the load placed on the lumbar spine during bending, lifting, and rotation, all activities that commonly aggravate disc injuries.
6. Addressing Fear and Guarding
Many patients hold their breath, brace excessively, or avoid bending entirely. Flora teaches safe, confident movement strategies that restore normal function and reduce the fear-avoidance cycle that can otherwise prolong recovery.
7. Shockwave Therapy for Associated Problems
Shockwave therapy is not applied directly to discs, but many people with disc injuries can also develop gluteal tendinopathy or chronic muscle tightness. In these cases, shockwave therapy can effectively address these secondary issues alongside the main rehabilitation programme.
Quick Tip: If your back locks or your leg symptoms worsen after sitting for long periods, note what you were doing before symptoms flared. This pattern information is invaluable during assessment and helps identify your directional preference more quickly.
How Long Does Recovery Take?
Recovery timelines vary depending on the severity of disc involvement and whether nerve symptoms are present:
- Mild disc irritation: significant improvement within 2-6 weeks
- Moderate disc involvement: 6-12 weeks with consistent rehabilitation
- Persistent nerve symptoms: 12 weeks or more, as nerve tissue heals more slowly than muscle or joint tissue
Nerves do heal, though they do so gradually. Consistent, well-guided rehabilitation throughout this period makes a measurable difference to the overall outcome.
Can Disc Bulges Return?
They can recur, but most people recover fully and return to normal life without ongoing problems. Long-term success depends on maintaining:
- Good spinal and hip strength
- Adequate mobility
- Healthy movement habits
- Confidence with bending, lifting, and daily activities
Avoiding movement indefinitely is not the answer. Returning to full activity, with appropriate guidance, is the goal.
When to Book an Assessment
Seek an assessment with our physiotherapy team if any of the following apply:
- Pain has lasted longer than one week
- Leg pain is worse than your back pain
- You are experiencing numbness or tingling
- Sitting is painful or difficult to sustain
- Your back locks frequently
- You feel unsure how to move safely
Early, accurate assessment often shortens overall recovery considerably. If you have concerns about your symptoms, do not wait.
Frequently Asked Questions
Is a disc bulge the same as a slipped disc?
“Slipped disc” is a commonly used term, but it is not anatomically accurate. Discs do not slip out of place. A disc bulge or herniation describes a change in the disc’s shape or a displacement of its inner material, not a disc that has moved entirely. The term is misleading and often causes unnecessary alarm.
Do I need an MRI before starting physiotherapy?
In most cases, no. A thorough clinical assessment can guide treatment effectively without imaging. MRI findings often do not correlate directly with symptoms, and many people with disc changes visible on MRI have no pain at all. Your physiotherapist will advise if imaging is genuinely warranted.
Can I exercise with a disc herniation?
Yes, with appropriate guidance. Staying active is generally beneficial and supported by current research. The key is identifying which movements reduce your symptoms and which aggravate them. Your physiotherapist will help you find safe exercise options from the very first session.
How is sciatica related to disc herniation?
Sciatica refers to pain that travels along the sciatic nerve, typically from the lower back into the buttock and down the leg. A disc herniation is one of the most common causes, as the displaced disc material can irritate or compress the nerve root. The majority of sciatica cases arising from disc herniation resolve well with physiotherapy.
What are the warning signs that I need urgent medical attention?
Seek immediate medical attention if you experience loss of bowel or bladder control, numbness in the saddle area (inner thighs and groin), or rapidly progressive weakness in both legs. These symptoms may indicate cauda equina syndrome, which requires emergency assessment. This condition is uncommon but must not be delayed.
How many physiotherapy sessions will I need for a disc herniation?
This depends on the severity of the disc involvement and whether nerve symptoms are present. Mild cases often show significant improvement within a few weeks. More complex cases with persistent nerve involvement may take three months or longer. Flora will give you a realistic timeframe based on your individual assessment findings.